If you are looking for health coverage and you do not have it through an employer, three options come up almost immediately: Medicaid, the Children’s Health Insurance Program known as CHIP, and marketplace plans purchased through the Health Insurance Marketplace. All three exist to make coverage more accessible, but they serve different populations, have different costs, and work in fundamentally different ways. Knowing the distinctions helps you figure out which one actually fits your household situation right now.
How Medicaid and CHIP Work
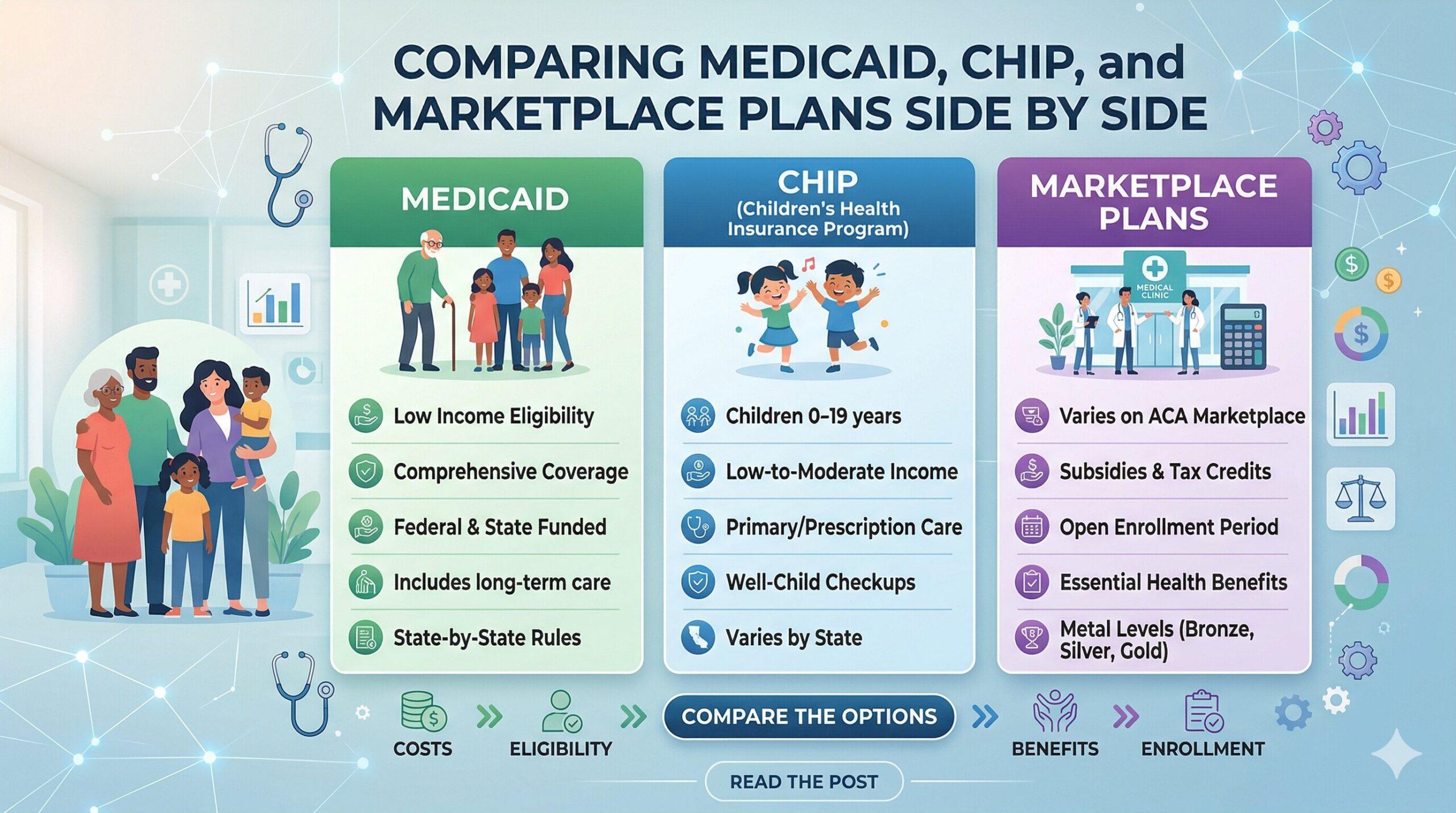
Medicaid is a joint federal and state program that provides free or very low-cost health coverage to adults and families with low incomes. Since the Affordable Care Act expanded Medicaid eligibility, most states now cover adults earning up to 138 percent of the federal poverty level. Coverage is comprehensive and typically includes doctor visits, hospital stays, mental health services, prescription drugs, and preventive care. There are no monthly premiums in most states for people who qualify, and cost-sharing is minimal. Eligibility is based on current income, so you can apply at any time of year, not just during open enrollment.
CHIP is specifically for children in families that earn too much to qualify for Medicaid but cannot afford private insurance. In most states, CHIP covers children up to age 19 in families earning up to 200 percent of the federal poverty level, and some states set that threshold even higher. The program covers routine checkups, immunizations, emergency care, dental and vision services, and prescriptions at very low or no cost. Like Medicaid, CHIP enrollment is open year-round, which means you can apply whenever you realize your child is eligible. One thing many families do not know is that children may qualify for CHIP even when the parents themselves do not qualify for any public coverage, making it possible to have adults on a marketplace plan and children on CHIP simultaneously.
Where Marketplace Plans Fit and Who They Serve
Marketplace plans are for people who do not qualify for Medicaid or CHIP and do not have access to affordable employer-sponsored coverage. These plans are purchased through the federal marketplace at HealthCare.gov or through state-run exchanges. The key financial benefit is the premium tax credit, which reduces your monthly premium based on your household income and size. Households earning between 100 and 400 percent of the federal poverty level qualify for subsidies, and recent legislative changes have extended enhanced credits beyond that range for many households.
The main practical difference between marketplace plans and Medicaid is cost and provider choice. Marketplace plans have monthly premiums even after subsidies, along with deductibles, copays, and out-of-pocket maximums. They offer more provider choice in most cases and have structured plan tiers from Bronze through Platinum that let you balance monthly costs against out-of-pocket exposure. The right choice between these three options depends almost entirely on your household income and your state’s Medicaid expansion rules.
One comparison that matters practically is how quickly coverage starts once you apply. Medicaid and CHIP can often be backdated to cover medical expenses from the month you applied. Marketplace coverage typically begins on the first of the month following enrollment. For someone who needs care urgently, this timing difference matters significantly. The simplest starting point for any household navigating these options is the eligibility screener at HealthCare.gov, which screens for Medicaid and CHIP eligibility automatically before presenting marketplace plan options, preventing the common mistake of purchasing a marketplace plan when you would have qualified for free Medicaid coverage instead.One additional dimension worth understanding is what happens to your coverage when your income changes during the year. Medicaid eligibility is based on current monthly income, which means a significant income increase can make you ineligible mid-year and require a transition to a marketplace plan. Both Medicaid and marketplace plans have specific processes for reporting mid-year changes, and using them promptly rather than waiting until annual renewal is always the better approach.



Leave a Reply